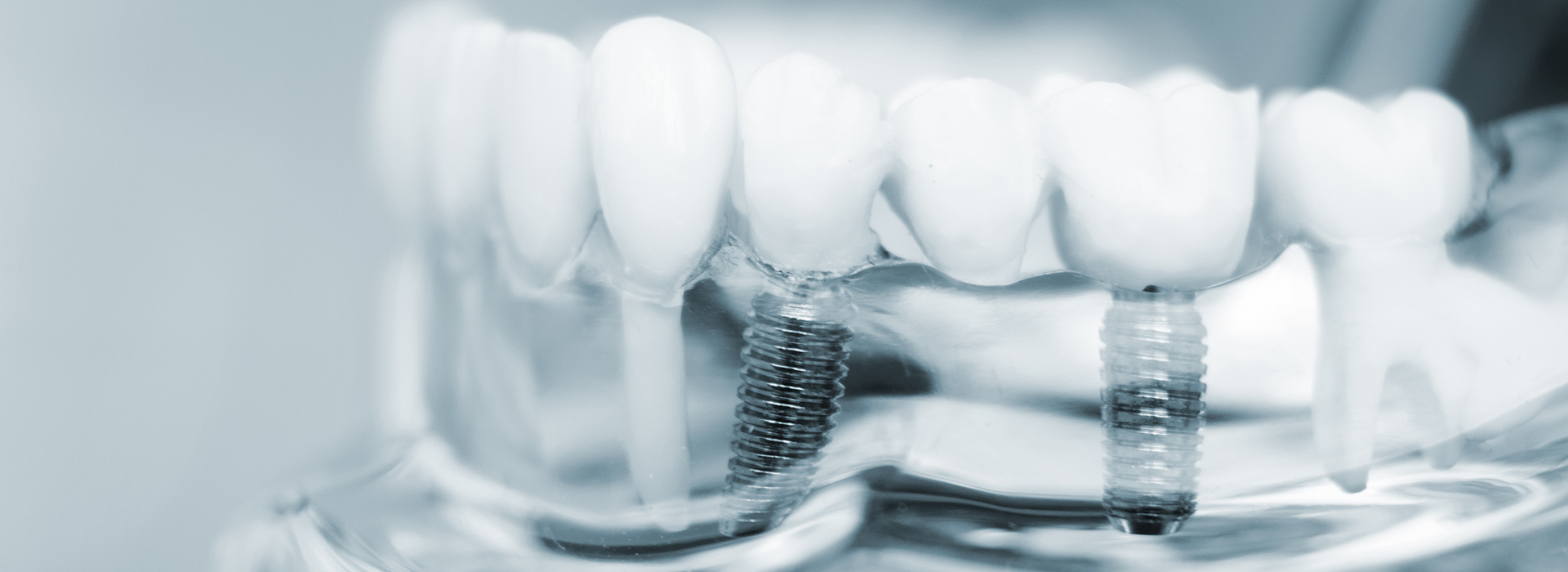
Missing teeth change more than your smile — they alter how you eat, speak, and how your face holds its shape. Dental implants are designed to recreate both the visible tooth and the unseen root, giving you a restoration that behaves like natural dentition. With thoughtful planning and modern materials, implants can restore chewing efficiency and help preserve the bone and soft tissue around a missing tooth.
Implants are suitable for a wide range of situations, from replacing a single tooth to supporting full-arch prostheses. The goal is consistent: rebuild function, protect neighboring teeth, and deliver an appearance that blends with your natural smile. In many cases implants offer advantages over removable options because they remain fixed and stable during everyday activities.
At Amaya Dental, our approach begins with understanding each patient’s goals and medical history so that treatment recommendations are personalized. We prioritize clear explanations so you know what to expect from evaluation through final restoration. That combination of clinical care and communication helps patients feel confident about choosing implants when they are the right solution.

A dental implant is a biocompatible post — typically made from titanium or a titanium alloy — that is placed into the jawbone to act as an artificial tooth root. Over a period of weeks to months the bone cells grow to the surface of the implant in a process called osseointegration. Once that integration is stable, the implant can support a crown, bridge, or denture with long-term predictability.
This root-form design is what distinguishes implants from other tooth replacement options. Because they anchor directly to bone, implants restore force transmission when you bite and chew, which helps maintain bone volume and supports surrounding tissues so your face keeps its natural contours.
Modern implant systems and prosthetic materials allow us to match the color, shape, and texture of adjacent teeth. The restorative phase focuses on creating a comfortable, natural-looking crown or denture that harmonizes with the rest of your smile while delivering reliable function.
Implant treatment is not one-size-fits-all. Depending on how many teeth are missing and the condition of your jawbone, options range from a single implant with a crown to implant-supported bridges and full-arch restorations. Each approach has different planning considerations, surgical steps, and timelines, but all aim to restore a stable, comfortable bite and a pleasing esthetic outcome.
For patients who have worn dentures for years, implant-retained or implant-supported solutions can greatly improve stability and confidence. For those missing a single tooth, an implant-supported crown avoids altering neighboring teeth the way a traditional fixed bridge might. The selection is driven by functional needs, long-term health of the mouth, and your personal priorities.
Planning usually begins with a comprehensive exam and imaging to assess bone volume and the relationship of nearby anatomic structures. From there, we map implant positions to optimize support, esthetics, and ease of future hygiene — all essential to a durable outcome.
Placing an implant is considered a minor surgical procedure and is most often performed in an outpatient setting. The initial visit typically includes a review of your medical history, diagnostic imaging, and a discussion about anesthesia or sedation options to ensure comfort. Thoughtful planning minimizes surprises and helps create a predictable timeline for care.
Following placement, implants require time to integrate with the jawbone. During that healing period you may wear a temporary restoration that protects the site and maintains esthetics. We provide clear postoperative instructions and schedule follow-ups to monitor healing and adjust care when needed.
Once integration is confirmed, the restorative phase begins: impressions or digital scans capture the exact position of the implants so we can design crowns, bridges, or dentures that fit precisely. Properly placed and maintained implants can function reliably for many years, so ongoing hygiene and routine dental visits are key to long-term success.
Dental implants offer several clinical advantages: they restore chewing power, preserve bone, and prevent the shifting of adjacent teeth. Because implants do not rely on neighboring teeth for support, they often preserve the health of surrounding natural dentition. Additionally, implants eliminate many of the stability issues associated with removable dentures.
That said, not every mouth is immediately ready for implant placement. Sufficient bone volume and healthy soft tissues are important for predictable results. When bone is deficient, grafting procedures can rebuild the foundation needed to support an implant. Smoking, certain systemic conditions, and untreated periodontal disease can affect healing, so these factors are carefully evaluated as part of treatment planning.
Modern diagnostics and techniques — including three-dimensional imaging and guided surgical planning — increase the accuracy of implant placement and can simplify complex cases. These technologies allow us to anticipate challenges, reduce chair time, and place implants in positions that support both form and function.
For a single missing tooth, an implant topped with a custom crown restores the tooth without altering neighboring teeth. The result looks and functions like a natural tooth and simplifies oral hygiene compared with a three-unit bridge.
When several adjacent teeth are missing, an implant-supported bridge can replace the teeth without relying on the surrounding natural dentition. Strategically placed implants support a span of crowns and maintain the bone in the areas that matter most for facial support.
For patients missing most or all teeth in an arch, full-arch restorations using four to six implants provide a fixed, non-removable solution that behaves much like natural teeth. Alternatively, implant-retained dentures attach to a smaller number of implants to significantly increase stability while remaining removable for cleaning.
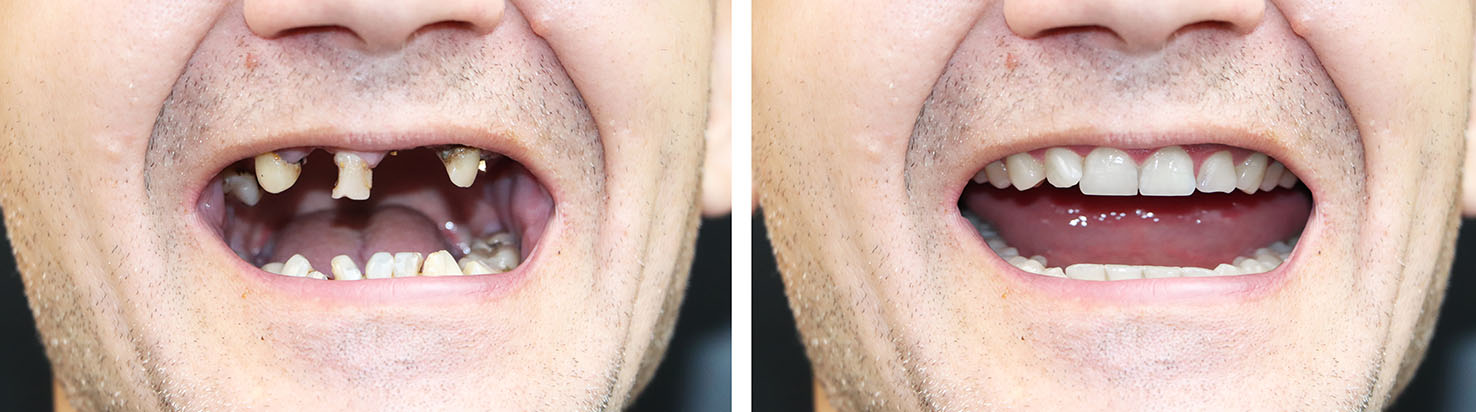
Because implants need solid bone to support them, various preparatory procedures can be part of a comprehensive plan. Bone grafting rebuilds areas where volume has been lost due to extractions, periodontal disease, or long-term tooth loss. Socket preservation and guided bone regeneration are common techniques used to create a stable foundation.
Sinus augmentation can be necessary in the upper jaw when the sinus floor limits implant length. Soft tissue grafting may also be recommended to improve the quality and thickness of gum tissue around the implant, which contributes to a natural-looking margin and easier hygiene.
These adjunctive procedures extend the scope of what is treatable with implants and are performed when they increase the likelihood of a durable and esthetic result. Our team will explain the rationale for any additional steps and include them in your personalized plan only when they are clinically indicated.
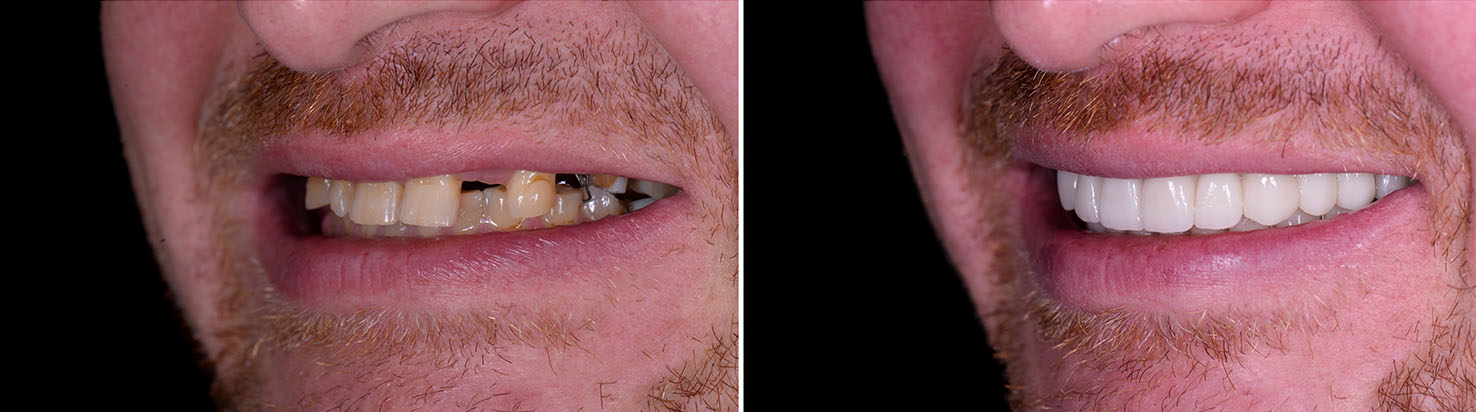
Successful implant dentistry combines surgical skill, prosthetic expertise, and thoughtful planning. Look for providers who use modern diagnostic tools, communicate clearly about options, and tailor treatment to each patient’s needs. A collaborative approach — where surgical and restorative phases are coordinated — produces the best outcomes.
Our team focuses on careful evaluation, evidence-based techniques, and open discussion so you can choose the restorative path that fits your priorities. We balance durability, esthetics, and long-term oral health in every plan we create.
If you’d like to learn more about implant dentistry or explore whether implants are the right solution for you, contact us for more information. We’re happy to review your situation, explain the steps involved, and outline what to expect next.
A dental implant is a biocompatible post, most commonly titanium, that is surgically placed into the jaw to serve as an artificial tooth root. Over weeks to months the surrounding bone integrates with the implant in a process known as osseointegration, creating a stable foundation for a restoration. Once integrated, the implant can support a crown, bridge, or denture and restore normal biting and chewing function.
Because implants anchor directly to bone they help preserve bone volume and maintain the facial contours that support a natural appearance. Modern restorative materials and laboratory techniques allow restorations to match the color, shape, and texture of adjacent teeth. The overall goal is to combine reliable function with an esthetic result that simplifies hygiene and daily care.
Good candidates for dental implants are adults in generally good health with adequate jawbone to support an implant or with the willingness to undergo preparatory procedures such as bone grafting. Chronic conditions like diabetes or habits such as smoking can affect healing, so these factors are reviewed and managed as part of the evaluation. Untreated periodontal disease should be controlled before implant placement to reduce the risk of complications.
When bone volume is insufficient, grafting, socket preservation, or sinus augmentation can often rebuild the foundation needed for predictable implant placement. Advanced imaging and careful planning expand candidacy for many patients who were previously told implants were not an option. At Amaya Dental our team evaluates medical history, oral health, and patient goals to recommend the most appropriate and evidence-based path forward.
The overall length of implant treatment varies with the case and the chosen approach, with common timelines ranging from a few months to longer when additional procedures are required. Initial evaluation and any preparatory treatments such as grafting add time before implant placement, and the implant then typically requires a healing period to integrate with the bone. Some systems and protocols allow for immediate provisional restorations, but the final prosthetic phase waits until integration is confirmed.
Once healing is complete, restorative appointments involve precise impressions or digital scans to fabricate crowns, bridges, or dentures that fit the implants accurately. Computer-guided planning and modern prosthetic workflows can reduce surgical time and improve predictability, but the final schedule is individualized. Your clinician will provide a clear sequence of visits and milestones during the planning visit so you know what to expect.
Implant placement is typically performed as an outpatient procedure under local anesthesia with options for oral or IV sedation when appropriate to enhance comfort. The surgical visit involves careful tissue management and precise placement of the implant into the prepared bone site, often guided by preoperative imaging or a surgical guide. Most patients experience routine postoperative symptoms such as swelling and mild discomfort that are managed with short-term medications and cold therapy.
During the initial healing phase you may receive a temporary restoration to maintain esthetics and function while the implant integrates with the bone. Follow-up visits are scheduled to monitor healing and to remove sutures or adjust the temporary as needed. Once osseointegration is confirmed, the restorative phase begins and the final prosthetic is delivered with instructions for long-term care.
Comprehensive planning is the foundation of predictable implant dentistry and begins with a detailed medical and dental history plus clinical examination. Three-dimensional imaging such as cone-beam computed tomography (CBCT) and high-quality digital radiographs are commonly used to evaluate bone volume, anatomic landmarks, and the relationship of adjacent teeth. These diagnostic tools allow clinicians to visualize the proposed implant position and to anticipate potential challenges before surgery.
Digital planning software enables virtual placement and the fabrication of surgical guides that translate the plan accurately to the clinic, improving safety and efficiency. Collaboration between the surgical and restorative teams ensures the implant position will support an esthetic and hygienic final restoration. This coordinated workflow helps reduce surprises and supports long-term success.
Implant restorations range from a single crown to implant-supported bridges and full-arch solutions depending on how many teeth are missing and the patient’s goals. A single implant with a custom crown replaces one tooth without altering neighboring teeth, while implant-supported bridges can span multiple missing teeth without relying on adjacent natural dentition. For patients missing an entire arch, fixed full-arch restorations using four to six implants or implant-retained dentures provide stable options that restore function and esthetics.
The choice between fixed and removable prosthetics depends on factors such as bone quantity, desired maintenance routine, and the need for retrievability. Technologies such as CAD/CAM manufacturing, zirconia frameworks, and screw-retained designs improve fit and simplify repairs. Your clinician will discuss the restorative options and their implications for hygiene and long-term care when developing your personalized plan.
As with any surgical procedure, implant therapy carries potential risks including infection, delayed healing, implant failure, and, rarely, injury to adjacent nerves or the sinus. Thorough preoperative evaluation, sterile surgical technique, and careful follow-up reduce the likelihood of complications. Risk factors such as smoking, uncontrolled systemic disease, and poor oral hygiene are addressed during planning to improve outcomes.
If complications arise, they are managed with evidence-based interventions such as local debridement, antibiotics when indicated, bone grafting or revision surgery, and, in rare cases, implant removal and staged retreatment. Early detection through scheduled follow-ups allows the team to intervene quickly and minimize long-term effects. Open communication about signs to watch for and prompt reporting of concerns help the care team respond effectively.
Long-term success of implants depends on daily home care and regular professional maintenance much like natural teeth. Patients should brush twice daily, use interdental brushes or floss designed for implants, and avoid tobacco to support gum health and reduce the risk of peri-implant disease. Routine dental visits allow clinicians to remove plaque and calculus that can accumulate around implant restorations and to check the prosthetic components.
In addition to hygiene, monitoring occlusion and using protective appliances such as night guards when needed can prevent excessive forces that compromise implant integrity. Professional examinations typically include radiographic assessment and evaluation of soft tissue health to detect early changes. A maintenance schedule tailored to the individual’s risk factors helps protect the investment in implant therapy over the long term.
Beyond replacing a missing tooth, dental implants play a role in preserving bone and supporting the surrounding oral structures, which can help maintain facial contours and oral function. By restoring proper force transmission during chewing, implants reduce the likelihood of neighboring teeth drifting into space and help maintain a stable bite. Improved function can also aid in comfortable eating and clear speech when compared with some removable options.
Implants can be integrated into comprehensive restorative plans that address multiple functional and esthetic needs, including long-term oral health goals. Careful coordination between surgical and restorative clinicians allows implants to support broader treatment outcomes such as balanced occlusion and durable prosthetics. Patients considering implants should discuss how the treatment fits into their overall oral health plan during the consultation visit.
Choosing a provider for implant dentistry involves evaluating surgical experience, restorative expertise, and the use of modern diagnostics and technologies such as CBCT and digital planning. Look for a clinician or team that explains risks and benefits clearly, coordinates surgical and prosthetic phases, and provides a documented treatment plan that addresses both function and esthetics. Contacting a practice to discuss their workflow and to review how they manage complex cases can help you assess whether their approach aligns with your needs.
At Amaya Dental our team emphasizes collaborative planning, evidence-based protocols, and clear communication to guide patients through the implant process from evaluation to final restoration. Asking about follow-up care, maintenance protocols, and how the team handles unexpected findings during treatment will give you a fuller picture of the support you can expect. A thoughtful provider will prioritize predictable outcomes and long-term oral health when recommending implant solutions.
Quick Links