
Dental extraction is a carefully considered treatment — never a first resort. Our goal is always to preserve natural teeth whenever possible, but sometimes removing a tooth is the safest path to preserve oral health, comfort, and function. When that choice is made, we focus on clear communication, thoughtful planning, and minimizing discomfort every step of the way.
At Amaya Dental, we approach each extraction as part of a larger treatment plan tailored to your unique needs. That begins with a thorough review of your medical and dental history, a clinical examination, and the appropriate diagnostic imaging. Those steps help our clinicians determine whether removal is necessary and which technique will give the best outcome.
We understand that the thought of an extraction can be stressful. Our team emphasizes patient comfort, explaining the procedure in plain language and reviewing options such as local anesthesia and dental sedation when appropriate so you can make an informed decision with confidence.
Primary (baby) teeth that don’t shed on schedule
Sometimes a primary tooth remains firmly attached after the permanent tooth begins to erupt. When the baby tooth’s root fails to resorb or it becomes fused to the jawbone, it can block normal development and alignment. Timely removal can prevent orthodontic complications and guide a healthier eruption pattern for the permanent tooth.
Extensive decay where restoration is no longer viable
Decay that has progressed beyond repair can compromise both the structure and the nerve of a tooth. When there is insufficient healthy tooth left to support a restoration, extraction is the treatment that protects surrounding teeth and adjacent tissues from further infection.
Severe fractures or damage to a tooth
Cracks and fractures come in many forms. If a fracture extends beneath the gum line or into the root in a way that precludes reliable restoration, removing the tooth may be the best option to prevent pain and ongoing problems.
Advanced periodontal disease affecting support structures
Periodontal disease that significantly weakens the bone and soft tissues around a tooth can leave it mobile and nonfunctional. When supportive structures cannot be restored to a healthy state, extraction may be necessary to stop the spread of infection and preserve oral function.
Wisdom teeth that are impacted, decayed, or misaligned
Third molars often lack sufficient space to erupt properly. Impacted or poorly positioned wisdom teeth can damage neighboring teeth, cause crowding, or develop infections that affect adjacent tissues. Removing problematic wisdom teeth can prevent future complications and maintain overall oral health.
Teeth removed to facilitate orthodontic treatment
Orthodontic plans sometimes require the strategic removal of one or more permanent teeth to create room for alignment and to achieve a balanced bite. When extraction is part of the recommended orthodontic approach, it is coordinated closely with the orthodontist to support predictable results.
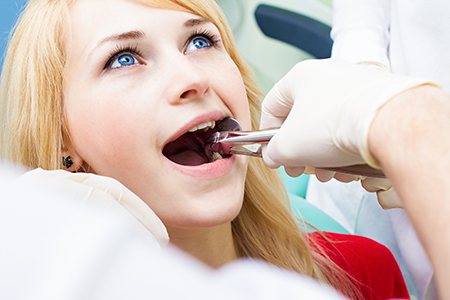
Before recommending removal, we gather the information needed for a safe, predictable procedure. This includes a review of your health history, current medications, and any conditions that could affect healing. We also discuss your comfort preferences so we can plan appropriate anesthesia or sedation options.
Diagnostic imaging is an essential part of planning. Digital radiographs provide detailed views of tooth roots, surrounding bone, and the relationship to important anatomical structures. Those images help us decide whether a simple extraction is sufficient or whether a surgical approach — sometimes requiring referral to an oral surgeon — is the safest path.
We will explain any pre-procedure instructions, such as medication adjustments or temporary medical clearances, when needed. Clear preoperative guidance reduces risk and supports a smoother recovery, and we encourage you to ask questions so you understand each step before the appointment.
A simple extraction is performed when the tooth is fully visible and the root anatomy allows straightforward removal. After numbing the area with a local anesthetic, the tooth is gently loosened and removed using instruments designed to preserve surrounding bone and tissue. The process is efficient and generally has a quick recovery time.
Surgical extractions are indicated for teeth that are broken at the gumline, impacted, or fused to the bone. In these cases, the dentist or an oral and maxillofacial surgeon makes a small incision in the gum and may remove a bit of bone to access and remove the tooth safely. Local anesthesia is provided, and sedation options can be arranged to reduce anxiety and discomfort.
When a surgical approach is recommended, we discuss the reasons for referral, what the procedure will involve, and the expected timeline for healing. Our focus is on minimizing risk while achieving the best long-term outcome for your oral health.
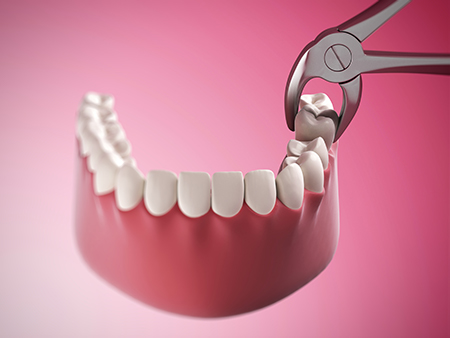
Recovery after an extraction follows a predictable course, and most patients heal without complications when they follow straightforward care steps. We provide tailored post-operative instructions that address pain control, swelling management, and activity restrictions to support efficient healing.
It is normal to experience some bleeding, swelling, and mild discomfort in the first 24–48 hours. With rest, recommended medications, and simple home care, these symptoms typically improve quickly. Proper wound care and avoiding habits that disturb the clot — such as rinsing vigorously or using a straw — help prevent complications.
If stitches are used, we will tell you whether they are dissolvable or need removal at a follow-up visit. We also let you know what signs warrant a call to the office, including persistent heavy bleeding, increasing pain, fever, or other unexpected symptoms.
Manage initial bleeding with firm gauze pressure
Bite gently on the provided gauze for the recommended intervals to encourage clot formation. Replace the gauze as instructed and contact the office if bleeding remains heavy beyond the expected time frame.
Protect numb tissues until sensation returns
Avoid chewing or touching the surgical area while local anesthesia is active to prevent accidental injury to lips, cheeks, or tongue.
Take prescribed medications as directed
If antibiotics or pain medications are prescribed, follow the dosing instructions exactly. Over-the-counter analgesics may also be recommended for mild discomfort; take them according to the guidance provided.
Avoid actions that disturb the healing clot
Refrain from spitting, rinsing vigorously, or using straws for the first 24 hours. These activities can dislodge the clot and increase the risk of a painful condition called dry socket.
Control swelling with brief ice application
Apply an ice pack externally near the treated area for short intervals during the first day to reduce swelling. After 24 hours, warm compresses can help relieve residual discomfort if advised.
Refrain from smoking
Tobacco use interferes with clot formation and wound healing; avoid smoking and other tobacco products for at least a week after surgery to support recovery.
Choose soft, nutritious foods
Start with cool, soft items and avoid hot, spicy, or carbonated foods and beverages for the first day or two. Staying well-hydrated supports overall healing.
Maintain gentle oral hygiene
Brush carefully around the extraction site and use a mild saltwater rinse after the first 24 hours if recommended. Avoid vigorous mouthwashes that can irritate the healing tissue.
Attend follow-up appointments
Keep any scheduled visits so we can monitor healing, remove sutures if necessary, and review options for replacing the extracted tooth when appropriate.
Contact the office promptly if you notice unusual symptoms such as severe pain that intensifies after the first few days, excessive swelling, or persistent fever. Early evaluation helps us address issues quickly and reduce the risk of complications.
Removing a tooth often prompts a conversation about how to restore chewing function, prevent drifting of neighboring teeth, and maintain facial structure. Replacement can be planned immediately or after a short healing period, depending on the clinical situation and the chosen restorative option.
Common replacement choices include removable dentures, fixed bridges, and dental implants. Each has distinct advantages and considerations related to durability, maintenance, and how closely it replicates natural teeth. We will discuss the timing and sequence of care so your replacement integrates into a practical, long-term plan for oral health.
When appropriate, we coordinate with specialists and use diagnostic tools to evaluate bone volume, soft tissue condition, and the overall treatment timeline. This collaborative planning helps ensure predictable function and aesthetics once the replacement is in place.
Our clinicians combine clinical expertise with modern diagnostic tools to make extractions as safe and comfortable as possible. From precise imaging to gentle surgical technique and thoughtful aftercare instructions, attention to detail guides every phase of treatment.
We tailor sedation and pain-control options to individual needs, helping anxious patients tolerate procedures with minimal stress. When a case exceeds in-office scope, we coordinate referrals to oral surgeons and remain involved in post-operative planning so care is seamless.
Throughout treatment, the focus is on transparency and respect. We explain the rationale behind recommendations, outline what to expect during recovery, and present appropriate options for restoring function and appearance when a tooth is removed.
In summary, extraction can be a necessary step in maintaining or restoring oral health when a tooth is compromised. With careful evaluation, thoughtful planning, and attentive aftercare, patients can expect safe treatment and predictable healing. Contact us for more information about extraction and restorative options — we’re here to help you make informed choices about your dental care.
The most common reasons for tooth loss include advanced periodontal disease, extensive tooth decay, and facial trauma. According to statistics, gum disease is responsible for close to 70% of tooth loss in adults. Although less frequent than the preceding three reasons, it should also be noted that specific diseases, drugs, smoking, and poor nutrition contribute to the risk of tooth loss.
The Centers for Disease Control and Prevention report that in the United States, an average of 12 teeth (including the wisdom teeth) are lost by the age of 50. Also, 26% of adults between 65 and 74 years of age have lost all their teeth.
Every patient and every situation is different. However, when a tooth and the surrounding tissues are numbed with a local anesthetic, you should only expect to feel a bit of pressure, but no pain as the tooth is being loosened from the surrounding tissues and extracted. For patients who are apprehensive and for some surgical extractions, our office will discuss our options in dental sedation to provide further relaxation and reduce any sense of discomfort.
While it's normal to feel some tenderness and swelling following an extraction, the degree of these sensations can vary. It mostly depends on the complexity of the extraction and the body's response to the procedure. We'll recommend or prescribe the appropriate pain medication to help ensure your comfort and give you specific instructions for maximum effectiveness and safety.
Typically, the recovery period following a simple extraction is shorter than a surgical extraction. However, a patient's overall health, habits, the size and location of the tooth, and other variables can influence recovery and healing. To speed up the recovery and avoid any complications, patients must follow the given at-home instructions diligently. We'll carefully review what to expect following your procedure and go over your post-op instructions.
Smoking interferes with blood clot formation, which is an essential first step in the healing process. Blood clot formation not only provides a protective layer to cover the underlying exposed bone and nerve endings, but it also supports the growth of new tissue. Cigarette smoke also contains chemical toxins that can disrupt the healing process and lead to problems such as continued inflammation, infection, or dry socket.
In a very small percentage of cases, a condition known as dry socket can develop in the aftermath of a dental extraction. This painful condition can arise when the blood clot in the extraction site doesn't form properly or gets dislodged. With dry socket, you may experience throbbing pain and symptoms such as bad breath and an unpleasant taste in your mouth. As skilled providers of care, our office will provide immediate treatment to alleviate your discomfort and promote healing.
The last teeth in your mouth to develop, wisdom teeth often do not have enough room to fully erupt or may be positioned in the wrong direction. These issues can affect your dental health as well as overall wellbeing. While some individuals never develop all their wisdom teeth, and a few have sufficient space for them, there are many people with partially or fully impacted third molars. Our office will monitor the development, position, and health of your wisdom teeth and will advise you if and when extractions are indicated.
After a tooth is removed, bone-grafting material is sometimes placed in the socket to promote healing and encourage new bone development. This procedure is often performed to support the eventual and successful placement of a dental implant.
At the office of Amaya Dental, we strive to make dental care affordable and accessible. Depending on the type or complexity of the extraction and other variables, the cost of the procedure can vary. Based on our diagnostic findings, our office will inform you of the healthiest choices in care, explain the fees, discuss insurance coverage, and explain your payment options.
Many dental plans offer some level of coverage for tooth extractions. We'll advise you if your plan covers the full cost of the procedure and if there is any out-of-pocket expense. Our business office will work with you to maximize your insurance benefits as much as possible while helping you minimize any out-of-pocket expenses.
A dental extraction is the clinical removal of a tooth from its socket in the jaw. Extractions are recommended when a tooth is severely damaged by decay or fracture, when advanced periodontal disease has compromised its supporting structures, or when a tooth obstructs proper dental development. The goal of extraction is to protect overall oral health and to eliminate sources of pain or infection that cannot be managed with conservative treatment.
Extractions are also used strategically in orthodontic care or to address problematic third molars that threaten neighboring teeth. Before proceeding, clinicians evaluate alternatives such as restorations, root canal treatment, or periodontal therapy to preserve natural dentition when feasible. When removal is the safest choice, the procedure is planned to minimize risk and support predictable healing.
Determining the need for extraction begins with a comprehensive review of your medical and dental history, a focused clinical exam, and diagnostic imaging such as digital radiographs. These steps reveal root shape, bone support, the extent of infection or decay, and the tooth's relationship to important anatomical structures, all of which influence the treatment recommendation. The clinician also weighs patient-specific factors like systemic health, medications, and long-term restorative goals before advising extraction.
When the situation is complex, the team discusses treatment options and explains why extraction may be preferable to restoration. In some cases a referral to an oral surgeon is recommended for advanced surgical removal or if specialized sedation is needed. Throughout this process, the emphasis is on clear communication so patients understand the rationale and planned sequence of care.
A simple extraction is performed on a tooth that is fully erupted and easily accessible in the mouth; it typically involves local anesthesia, gentle elevation, and forceps removal. Recovery from a simple extraction is usually straightforward with minimal postoperative discomfort and a relatively quick return to normal activities. This approach preserves surrounding bone and soft tissue when the root anatomy permits conservative removal.
Surgical extraction is indicated when a tooth is broken at the gumline, impacted, or has an unusual root configuration that requires additional access. The dentist or oral surgeon may make a small incision, remove a bit of bone, or section the tooth into pieces to remove it safely while protecting adjacent structures. Surgical cases often involve more detailed preoperative planning and may include sedation options to enhance patient comfort.
Wisdom teeth, or third molars, frequently lack sufficient space to erupt properly and can become impacted, misaligned, or partially erupted. These conditions increase the risk of infection, damage to adjacent teeth, cyst formation, and crowding, which is why clinicians commonly recommend removal when problems are present or likely to develop. Radiographic evaluation helps determine whether a wisdom tooth is likely to cause future complications or should be monitored.
Not all wisdom teeth require extraction; if they erupt fully, function normally, and are easily kept clean, they may be retained with routine monitoring. When removal is advised, timing is considered carefully to optimize healing and to coordinate with other dental treatments, such as orthodontics. The decision balances current symptoms, the tooth's position, and the patient's overall oral health needs.
Local anesthesia is the most common approach and numbs only the treatment area to allow a pain-free extraction while you remain awake and responsive. For patients with anxiety or for more complex surgical cases, additional options such as inhalation sedation (nitrous oxide), oral sedatives, or intravenous (IV) sedation may be offered to promote relaxation and comfort. The choice of anesthesia or sedation depends on medical history, anxiety level, procedure complexity, and patient preference.
Before selecting a sedation method, the dental team reviews your medical conditions and current medications to ensure safety and effectiveness. When deeper sedation or general anesthesia is needed, care may be coordinated with an oral surgeon or anesthesiologist. Clear preoperative instructions and post-procedure monitoring are provided to support a safe experience and smooth recovery.
Preparation begins with a review of your medical history and a list of current medications so the clinician can identify any factors that affect bleeding or healing. If sedation is planned, you may be instructed to fast for a specified period and arrange for a responsible adult to drive you home after the procedure. It is also helpful to plan for a short period of rest after the appointment and to have soft foods and any recommended supplies available at home.
Follow any specific preoperative instructions provided by the dental team, such as temporarily adjusting certain medications only under clinician guidance. Bring a list of questions to your appointment so you understand the planned technique, anesthesia choice, and expected recovery timeline. Clear communication before the procedure reduces surprises and supports a safer, more comfortable visit.
The first 48 hours commonly involve some bleeding, mild to moderate swelling, and controlled discomfort, which are normal parts of the early healing process. Biting gently on gauze as instructed helps form a stable clot and reduces bleeding, while brief cold compresses applied externally can limit swelling. Pain can usually be managed with prescribed or over-the-counter analgesics used according to the clinician's guidance.
Patients are advised to rest, avoid strenuous activity, and consume cool, soft foods during this period to protect the surgical site. Refrain from rinsing vigorously, spitting forcefully, or using straws for the first day to prevent clot disruption. If stitches were placed, the clinician will inform you whether they are dissolvable or require removal at a follow-up visit.
Preventing dry socket begins with protecting the blood clot that forms in the extraction site; avoid actions that create suction such as using straws, smoking, or vigorous rinsing for at least 24 hours. Maintain gentle oral hygiene around the area and follow any rinse schedule recommended by your clinician, typically starting with mild saltwater rinses after the first day. Proper medication adherence and following activity restrictions also support uncomplicated healing.
If you smoke or use tobacco products, stopping for at least a week after the extraction significantly reduces complication risks because tobacco interferes with clot formation and tissue repair. Watch for warning signs such as severe pain that intensifies several days after the procedure, foul odor, or visible bone in the socket, and contact the office promptly if any concerns arise. Early evaluation allows timely management and reduces the chance of prolonged healing problems.
You should contact the office if you experience persistent heavy bleeding that does not respond to gentle pressure, fever, uncontrolled swelling that worsens, or severe pain that increases after the first few days. Other reasons to call include allergic reactions to medications, unexpected discharge from the site, or any signs that your healing is not progressing as expected. Prompt communication allows the team to assess symptoms and provide interventions that prevent more serious complications.
For routine follow-up care, keep any scheduled appointments so the clinician can monitor healing, remove sutures if necessary, and review plans for tooth replacement when appropriate. If your procedure was performed by or referred to a specialist, the practice coordinates post-operative care and remains available to answer questions and manage recovery. Timely contact and follow-up support the best possible outcome.
Common replacement options include dental implants, fixed bridges, and removable dentures, each with distinct benefits related to function, longevity, and maintenance. The timing of replacement varies: immediate replacement may be appropriate in some cases, while others benefit from a short healing interval to allow soft tissue and bone to recover before definitive restoration. The clinician evaluates bone volume, tissue condition, and overall treatment goals to recommend the best path forward.
When implants are considered, diagnostic imaging and, if needed, bone grafting or site preparation are planned to ensure predictable long-term results. The team may coordinate care with specialists for complex reconstructions and will discuss the sequence of treatments so replacement integrates into a practical, long-term oral health plan. At Amaya Dental we help patients understand the clinical considerations and timing so they can make informed decisions about restoring function and appearance.
Quick Links