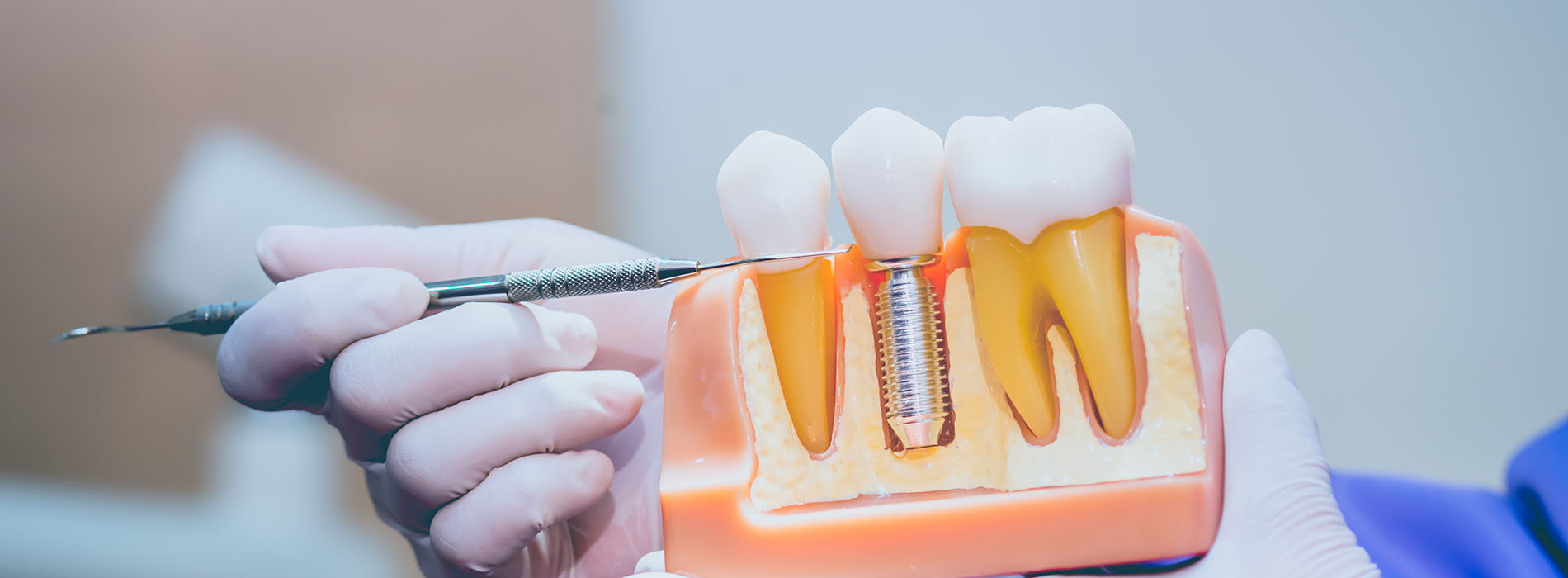
Implant restorations are the final, visible component that transforms a dental implant from a surgically placed post into a natural-looking replacement tooth. While the implant itself is a biocompatible titanium or zirconia fixture anchored in the jaw, the restoration is the crown, bridge, or denture that attaches to that foundation and restores chewing function, speech, and the appearance of a complete smile. When designed and placed correctly, restorations replicate the contours, color, and strength of natural teeth so patients can eat and speak confidently.
Patients often think of implants only as a way to replace missing teeth, but the restoration is equally important: it determines fit, comfort, and how closely the replacement resembles the surrounding dentition. A well-crafted restoration distributes chewing forces properly, protects the implant-abutment interface, and minimizes wear on adjacent teeth. Because restorations are custom-made, they are tailored to each patient’s bite, facial proportions, and aesthetic goals.
Modern implant restorations use digital planning, precision impressions, and lab-fabrication techniques to achieve consistent outcomes. The result is a stable, long-term solution that combines mechanical strength with a natural appearance. For patients considering implant-based tooth replacement, understanding the role of the restoration helps clarify expectations for function, maintenance, and long-term oral health.
While the aesthetic improvement of a full, even smile is an obvious benefit, implant restorations offer several functional and health-related advantages. By replacing the tooth root with an implant-supported restoration, bone loss in the jaw can be slowed or prevented because the implant transmits gentle stimulation to the bone much like a natural tooth root. This preservation of jawbone helps maintain facial structure and prevents the sunken appearance that can accompany missing teeth over time.
Restorations on implants also improve chewing efficiency compared with many removable options. Implant-supported crowns and bridges are fixed or securely attached, so they resist shifting and provide a stable bite. That stability can expand dietary options and make daily activities like speaking and smiling more comfortable and predictable for patients of all ages.
Finally, implant restorations are designed to protect surrounding teeth and soft tissues. Unlike traditional bridges that rely on adjacent teeth for support, implant restorations can stand independently, conserving healthy tooth structure. Properly contoured restorations also promote easier hygiene, which supports gum health and lowers the risk of peri-implant disease when patients follow recommended care routines.
The path to a finished implant restoration begins once the implant has integrated with the jawbone — a process called osseointegration. After this healing phase, the clinician assesses the implant’s stability and the health of surrounding tissues before proceeding. This checkpoint ensures the implant can reliably support the restoration long-term. Once cleared, the team moves forward with accurate impressions or digital scans to capture the position of the implant and the shape of the mouth.
Next, a customized abutment is selected or fabricated to connect the implant to its visible restoration. Abutments come in standard and custom options; choosing the right type influences the emergence profile, gum health, and final appearance. With the abutment in place, the dental laboratory crafts the crown, bridge, or overdenture using materials chosen for strength and aesthetics. Throughout this sequence, the dental team verifies that the restoration aligns with the patient’s bite and smile-line.
Before permanent attachment, temporary restorations may be used to test function and esthetics. These provisional pieces let patients experience how the final restoration will feel and allow clinicians to make adjustments. When both patient and provider are satisfied, the final prosthesis is secured — either cemented or screw-retained — and the team confirms proper bite, margins, and comfort to ensure a predictable, long-lasting result.
Implant restorations can be fabricated from a range of contemporary materials, each offering a balance of strength, translucency, and wear characteristics. Porcelain-fused-to-zirconia, monolithic zirconia, and layered ceramic options are commonly selected for their durability and lifelike appearance. Material choice is guided by the restoration’s location in the mouth, the patient’s bite forces, and aesthetic preferences — for example, anterior restorations may emphasize translucency and color matching while posterior restorations prioritize strength.
Design considerations extend beyond material. The restoration’s shape, occlusal scheme (how teeth contact), and the way it interfaces with the gum all influence longevity and comfort. Proper contouring of the restoration helps the patient maintain good hygiene and reduces the risk of soft tissue irritation. Additionally, clinicians consider whether a screw-retained or cement-retained approach is preferable; each has advantages for retrievability and soft-tissue management.
Precision in the manufacturing process — whether through CAD/CAM milling or skilled laboratory layering — matters for fit and esthetics. Tight tolerances at the implant-abutment-restoration junction reduce micro-movement and bacterial infiltration, both of which are important for long-term success. By combining thoughtful design with high-quality materials, clinicians create restorations that perform reliably while blending seamlessly with the patient’s natural smile.
Once an implant restoration is in place, routine care plays a central role in its longevity. Daily cleaning that includes brushing and flossing around the restoration is essential to control plaque and maintain healthy gum tissue. For many patients, specialized interdental brushes or floss threaders make it easier to clean beneath fixed bridges or around implant-supported crowns. Regular professional cleanings and check-ups allow the dental team to monitor tissue health and address minor issues before they escalate.
Patients should also be aware of behavioral factors that can affect restorations. Habits like nail-biting, chewing ice, or using teeth as tools can place undue stress on implant restorations. For individuals who grind or clench their teeth, the clinician may recommend a nightguard to protect both natural teeth and implant-supported restorations. Early attention to wear patterns, loose components, or changes in fit helps prevent more complex problems down the road.
Finally, open communication with your dental team ensures a proactive approach to maintenance. Periodic radiographs and clinical exams let clinicians evaluate bone levels, soft tissue health, and the condition of the restoration. With routine care and timely professional oversight, implant restorations can provide many years of dependable function and an attractive, natural-looking smile.
Selecting a dental team with experience in implant restorations makes a meaningful difference in outcomes. An experienced provider evaluates the entire mouth — bite dynamics, gum health, and opposing teeth — before recommending a restoration plan tailored to the patient’s needs. During the consultation, the clinician explains treatment steps, materials, and expected timelines so patients understand how the restoration will fit into their daily life and oral-health routine.
The clinical visit for a restoration often involves digital imaging or impressions, shade selection, and a review of the provisional restoration if one was placed earlier. Attention to detail in color matching, tooth shape, and margin fit ensures the final restoration looks natural and feels comfortable. A collaborative approach that considers patient preferences alongside clinical recommendations helps achieve a result patients are proud to wear.
At Amaya Dental, our goal is to combine modern techniques with individualized care so each restoration supports long-term health and confidence. When patients understand the process and their role in maintenance, implant restorations become a durable, life-enhancing solution for missing teeth.
In summary, implant restorations are the critical finishing touch that restore appearance, function, and oral health after implant placement. They require careful planning, precise fabrication, and ongoing care to perform well over time. If you would like more information about implant restorations or how they might fit into your treatment plan, please contact us for more information.
Implant restorations are the visible crowns, bridges, or dentures that attach to a dental implant and restore the form and function of missing teeth. They convert the implanted post into a usable tooth replacement that allows patients to chew, speak, and smile with confidence. Because restorations determine fit, appearance, and bite, they play an equal role to the implant fixture itself in long-term success.
A well-designed restoration distributes chewing forces properly and protects the implant-abutment connection from undue stress. Restorations also influence soft-tissue contours and hygiene access, both of which affect gum health around the implant. Understanding restorations helps patients set realistic expectations for appearance, maintenance, and function after implant therapy.
Dental implants are the biocompatible fixtures placed into the jawbone that act as artificial tooth roots, while implant restorations are the prosthetic teeth attached to those fixtures. The implant provides stability and bone stimulation, but the restoration provides the visible tooth surface and occlusal function. Both components must work together for a predictable outcome, yet they are planned and fabricated for distinct purposes.
The implant requires proper surgical placement and osseointegration before a restoration can be attached, and the restoration requires precise impressions or digital scans to achieve an accurate fit. Material choice, design, and connection type for the restoration are tailored to the implant’s position, the patient’s bite, and aesthetic goals. Coordinated planning between surgical and restorative teams reduces complications and improves long-term performance.
Implants can support single crowns, multi-unit bridges, and a variety of overdentures that are either fixed or removable. Single crowns replace individual teeth and are commonly used in anterior and posterior positions, while implant-supported bridges replace multiple adjacent teeth without relying on neighboring natural teeth. Overdentures can be anchored to several implants for improved stability compared with conventional removable dentures.
The choice of restoration depends on the number and location of missing teeth, the quality of the supporting bone, and the patient’s functional and aesthetic priorities. Each option has implications for maintenance, retrievability, and hygiene access, so clinicians evaluate the whole-mouth context when recommending a restorative approach. Custom abutments and advanced laboratory techniques help tailor each restoration to the patient’s needs.
Planning begins after the implant has integrated with the bone and includes clinical evaluation, digital imaging, and an accurate impression or scan of the implant’s position. The clinician determines the ideal emergence profile, occlusion, and tooth shape before selecting an abutment and restorative material. Digital workflows and CAD/CAM technology often streamline communication between the clinic and dental laboratory, improving fit and esthetics.
Laboratory fabrication can involve milling monolithic zirconia, layering porcelain over a framework, or crafting custom hybrid solutions depending on the case. Temporary restorations are sometimes used to test function and aesthetics before final delivery, allowing adjustments to be made early. Final restorations are secured either with screws or cement and are verified for margin fit, occlusion, and patient comfort during the insertion appointment.
Common materials include monolithic zirconia, layered zirconia, porcelain-fused-to-zirconia, and various high-strength ceramics designed to balance strength and esthetics. Material selection is guided by the restoration’s location in the mouth, the patient’s bite forces, and the need for translucency to match adjacent natural teeth. Posterior restorations often prioritize strength, while anterior restorations emphasize lifelike color and translucency.
Design considerations such as thickness, occlusal scheme, and connector size also influence the material decision, because they affect durability and wear behavior. The clinician and laboratory technician collaborate to select materials and finishing techniques that meet both functional demands and cosmetic expectations. Careful material choice reduces the risk of chipping, fracture, or excessive wear over time.
Screw-retained restorations are attached to the implant with a mechanical screw that allows for straightforward removal and retrieval when adjustments or repairs are needed. Cement-retained restorations are bonded to an abutment and may offer advantages in achieving ideal tooth position and esthetics when implant angulation is less favorable. Each method carries trade-offs related to retrievability, maintenance, and soft-tissue management.
Screw-retained designs reduce the risk of residual cement, which can contribute to soft-tissue inflammation, but they sometimes require small access holes that must be sealed cosmetically. Cement-retained restorations may deliver seamless margins in certain aesthetic situations but require meticulous cement removal and monitoring. Clinicians weigh retrievability, esthetic goals, and peri-implant tissue health when recommending one approach over the other.
Daily cleaning around implant restorations is essential and includes regular brushing and targeted interdental cleaning to remove plaque and food debris. Many patients benefit from soft interdental brushes, floss threaders, or specialized implant floss to reach beneath contours and between abutments, especially around multi-unit restorations. Gentle, consistent hygiene prevents biofilm buildup and supports the health of surrounding gums and bone.
Patients should avoid using teeth as tools, biting very hard objects, or chewing ice, all of which can stress restorative materials and components. Those who grind or clench their teeth should discuss a nightguard with their clinician to protect both natural teeth and implant-supported restorations. Promptly reporting looseness, unusual mobility, or discomfort helps the team address problems before they become more serious.
Regular dental checkups and professional cleanings are important for monitoring the condition of implant restorations and the health of peri-implant tissues. During these visits the dental team assesses occlusion, checks for wear or looseness, evaluates soft-tissue health, and may take periodic radiographs to monitor bone levels around the implant. Professional hygiene appointments also allow for removal of hard-to-reach deposits that at-home care may miss.
Maintenance intervals may vary depending on individual risk factors such as history of gum disease, smoking, or systemic health conditions, and the clinician will recommend an appropriate recall schedule. Maintenance may also include retightening screws, polishing restorative surfaces, or making minor adjustments to occlusion as needed. Proactive professional oversight helps extend the life of the restoration and preserves overall oral health.
Complications can include prosthetic issues such as loosened or fractured restorations, wear of restorative materials, and biologic concerns such as peri-implant mucositis or peri-implantitis. Mechanical problems are often repairable through component replacement, adjustment, or laboratory repair, while biologic complications require clinical management of inflammation, improved hygiene, and sometimes surgical intervention. Early detection through routine exams improves the likelihood of conservative treatment.
Addressing complications begins with a thorough diagnostic evaluation to identify the underlying cause, whether it is occlusal overload, residual cement, poor hygiene, or unmanaged systemic risk factors. Treatment plans may include professional cleaning, antibiotic protocols, soft-tissue management, or revision of the restorative design to improve hygiene access. A collaborative approach between the patient and dental team supports timely resolution and reduces the chance of recurrence.
Choose a provider who demonstrates experience with implant restorations and who evaluates the whole-mouth context, including bite dynamics, gum health, and opposing dentition. Look for a practice that uses modern imaging and laboratory communication workflows, and that explains materials, connection types, and maintenance expectations clearly. A thorough consultation that covers both surgical and restorative phases indicates a comprehensive approach to predictable outcomes.
At Amaya Dental our team emphasizes coordinated treatment planning and attention to detail to help ensure restorations perform well long term. Open communication about expected function, hygiene responsibilities, and follow-up care helps patients make informed decisions and supports durable results. Ask prospective providers about their restorative workflow, case planning, and how they handle maintenance and complications to find the best fit for your needs.
Quick Links