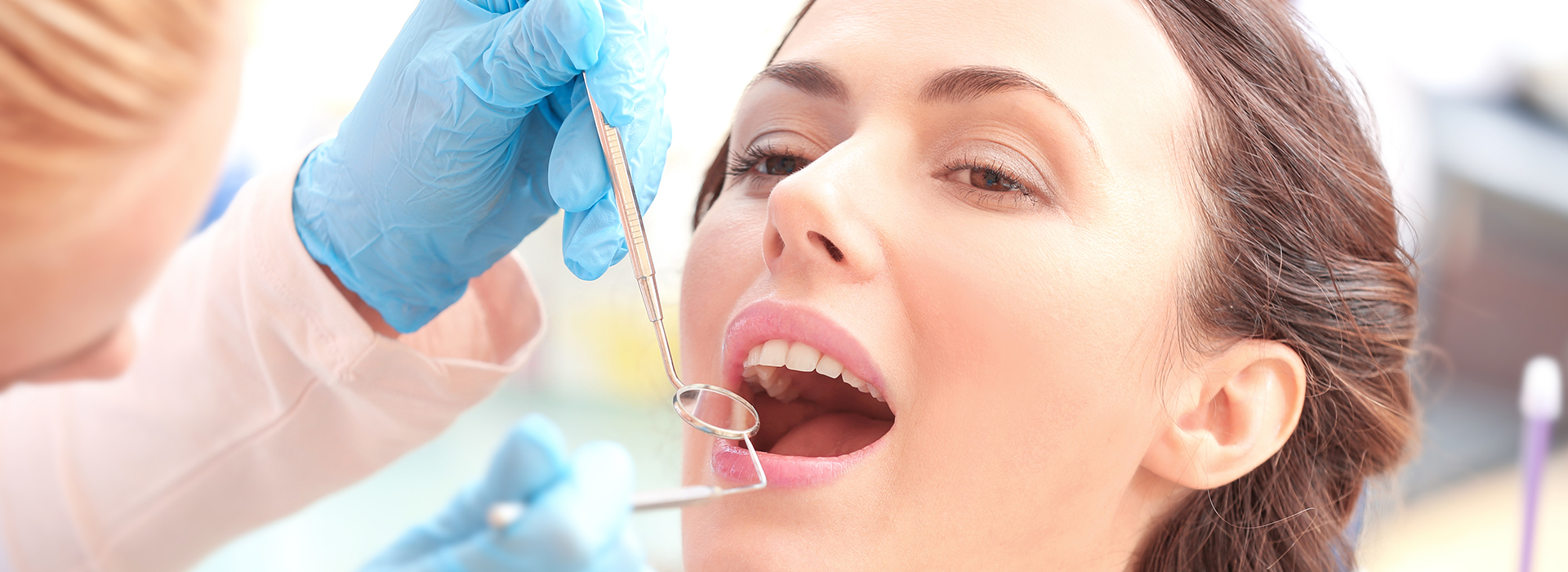
Gum disease is one of the most common chronic conditions affecting adults, and it’s the leading cause of tooth loss in later life. Roughly half of adults over 30 show signs of periodontal inflammation or damage, yet many people don’t recognize the early stages. At the office of Amaya Dental, we focus on clear explanations, practical prevention, and evidence-based treatment to help patients preserve healthy gums and lasting smiles.
Periodontal disease begins when bacteria in dental plaque irritate the gum tissue. Left unchecked, that irritation progresses from surface inflammation to deeper infection that can erode the fibers and bone that hold teeth in place. The process is driven by bacteria, the immune response, and environmental factors such as smoking, certain medications, and uncontrolled blood sugar.
Because early gum disease is often painless, visual and clinical signs are the most reliable clues. Regular dental exams and measurements of pocket depth tell us whether inflammation is limited to the gums or has reached supporting structures. Detecting trouble early makes treatment simpler and more predictable.
An informed patient who practices consistent home care and attends scheduled professional cleanings has the best chance of stopping disease before it causes permanent harm. When prevention fails, modern periodontal care offers a range of therapies designed to arrest progression and restore oral health.
Healthy gums anchor your teeth and provide a barrier against infection. When that barrier breaks down, oral bacteria can access deeper tissues and, in some cases, contribute to broader health issues. Research continues to explore links between periodontal inflammation and conditions such as diabetes, cardiovascular disease, and certain respiratory concerns.
Maintaining periodontal health supports everyday functions — eating, speaking, and smiling — while reducing the risk of costly and invasive procedures later on. Good gum care also preserves bone volume, which is essential should you ever need restorative work like implants or bridges.
Our approach emphasizes prevention and coordination with patients’ medical providers when systemic conditions complicate oral care. That collaborative mindset helps ensure periodontal treatment aligns with each patient’s overall health plan.
Early gum disease can be subtle. Common indicators include gums that redden or swell, bleeding during brushing or flossing, persistent bad breath, and increasing sensitivity around tooth roots. Patients may also notice changes in how their teeth fit together or a loose feeling in previously stable teeth — signals that deeper support has been affected.
These symptoms are not meant to alarm but to prompt evaluation. In many cases, addressing these signs quickly with improved hygiene and professional care can reverse the condition. Ignoring them allows pocketing and bacterial accumulation to worsen, making treatment more involved.
If you observe any of these changes, scheduling an exam allows for targeted diagnostics — probing depths, radiographs when appropriate, and a personalized treatment plan that reflects the severity and underlying causes of the problem.

Gingivitis is the earliest, and most treatable, form of gum disease. It shows up as tender, swollen, or bleeding gums without loss of bone or connective tissue. Because the supporting structures remain intact, gingivitis is a condition we can usually reverse with consistent professional and home care.
Professional cleanings to remove plaque and calculus, combined with improved brushing and interdental cleaning, often restore gum health in a matter of weeks. We also review oral hygiene techniques and suggest tailored tools to help patients maintain improvement.
Recognizing gingivitis as a warning sign is empowering: it means the problem has not yet caused permanent damage, and timely action can protect your teeth for the long term.

Periodontitis occurs when inflammation extends below the gumline and begins to destroy the fibers and bone that support teeth. As pocket depths increase, bacteria become harder to remove and the risk of tooth mobility and loss rises. This stage requires a more proactive treatment plan to preserve remaining tissues.
Treatment goals shift from reversal to stabilization and regeneration where possible. Care focuses on eliminating persistent bacterial deposits, reducing pocket depths, and supporting the body’s capacity to heal. In some cases, regenerative techniques can help restore lost bone and connective tissue.
With appropriate intervention and ongoing maintenance, many patients with periodontitis can maintain their teeth and enjoy improved function and comfort. Long-term success depends on both clinical therapy and a patient’s commitment to daily oral hygiene and professional checkups.
Periodontal care ranges from conservative, nonsurgical therapies to targeted surgical and regenerative procedures. The right plan depends on disease stage, the extent of tissue damage, and each patient’s medical history. Our team takes time to explain options, expected outcomes, and the sequence of care so patients can make informed decisions.
Noninvasive measures — including scaling and root planing, antiseptic rinses, and localized antimicrobials — are often the first line of treatment. These approaches reduce bacterial load, allow inflamed tissues to heal, and can significantly improve clinical measurements when performed with thorough home care.
Where deeper pockets or tissue loss persist, surgical techniques may be recommended to gain access for cleaning, reduce pocket depth, and, when appropriate, rebuild lost structures. Advances in laser therapy and regenerative materials have expanded our ability to treat complex cases with less discomfort and better healing.
In early or moderate disease, conservative therapy is effective and patient-friendly. Scaling and root planing — a careful cleaning of root surfaces beneath the gums — removes plaque and hardened deposits that fuel inflammation. Smoothing root surfaces helps new soft tissue attach and reduces spaces where bacteria can thrive.
Adjunctive measures such as localized antimicrobial agents or short-term systemic medications may be used selectively to enhance outcomes. These strategies are always paired with an individualized home-care plan and a schedule of professional maintenance visits to keep improvements on track.
When conservative care produces healthy pocket depths and stable tissues, patients can often transition to routine maintenance visits tailored to their risk level.
When pocket depths exceed what non-surgical methods can safely reach, surgical access may be necessary. Flap procedures allow clinicians to visualize and clean root surfaces and to recontour bone when needed. The result is reduced pocket depth and a more maintainable environment for daily hygiene.
Regenerative techniques — including guided tissue regeneration and bone grafting — aim to rebuild lost support in suitable cases. These procedures can improve stability, enhance smile aesthetics, and create a better foundation for restorative treatments when required.
Modern tools, such as dental lasers and microsurgical instruments, can reduce postoperative discomfort and promote faster recovery when indicated. Each surgical plan is customized to the patient’s anatomy, needs, and long-term goals.
Remove harmful bacteria and deposits from root surfaces and subgingival areas
Stabilize or rebuild bone and supporting tissues where damage has occurred
Reduce pocket depths to make daily cleaning effective and prevent recurrence
At Amaya Dental, our goal is to provide clear guidance and dependable periodontal care tailored to each patient’s situation. If you’re concerned about bleeding gums, persistent bad breath, or changes in tooth stability, contact us to learn more about how we can help preserve your oral health.
Periodontal disease, commonly called gum disease, is an inflammatory condition that affects the tissues supporting the teeth. It begins when bacterial plaque accumulates along the gumline and triggers an immune response that can damage soft tissue and bone. Early stages are often subtle, which is why regular evaluation is important for adults.
Progression depends on bacterial challenge, the body’s immune response, and risk factors such as smoking, certain medications, and uncontrolled blood sugar. Left untreated, inflammation can deepen into pockets that undermine tooth support and increase the risk of mobility and tooth loss. At Amaya Dental, we emphasize early detection and evidence-based care to preserve gum health and prevent long-term damage.
Early warning signs include gums that appear red or swollen, bleeding during brushing or flossing, persistent bad breath, and increased tooth sensitivity. Patients may also notice a change in how teeth fit together or a sensation that a tooth feels loose. Because early gum disease can be painless, these visible or symptomatic clues are important prompts to seek evaluation.
A clinical exam with periodontal probing and a review of medical history helps determine whether inflammation is limited to the soft tissue or has reached deeper support structures. Radiographs can reveal bone changes not visible on inspection alone. Prompt assessment allows for simpler, more predictable treatment when problems are detected early.
Gingivitis is the earliest and most treatable form of gum disease, characterized by tender, swollen, or bleeding gums without loss of bone or connective tissue. Because the supporting structures remain intact, gingivitis is usually reversible with consistent professional and home care. Professional cleaning combined with improved oral hygiene commonly restores gum health in weeks.
Periodontitis occurs when inflammation extends below the gumline and begins to destroy the fibers and bone that support teeth. This stage creates deeper pocketing where bacteria are harder to remove and increases the risk of tooth mobility and loss. Management shifts from reversal toward stabilization and, when appropriate, regeneration of lost tissues.
Periodontal assessment starts with a detailed clinical exam that includes probing pocket depths, checking for bleeding on probing, and recording attachment levels. A thorough medical and dental history identifies risk factors that influence treatment planning. These measures help determine whether inflammation is limited to the gingiva or involves deeper structures.
Radiographs are used to evaluate bone levels and identify patterns of bone loss; in select cases, advanced imaging such as CBCT may be recommended for complex planning. Periodontal charting over time documents progression or stability and guides maintenance intervals. Microbial testing or biopsy is used selectively when standard evaluation does not explain disease behavior.
Conservative therapies typically begin with scaling and root planing, a precise cleaning of root surfaces beneath the gums to remove plaque and calculus that fuel inflammation. Adjunctive measures can include localized antimicrobial agents and antiseptic rinses to reduce bacterial load. These approaches allow inflamed tissues to heal and often produce measurable improvement in pocket depths when paired with effective home care.
Short-term systemic medications may be considered selectively for patients with aggressive or rapidly progressing disease, always balanced against overall health considerations. Equally important is individualized instruction in brushing and interdental cleaning to maintain the benefits of in-office therapy. Following initial treatment, a tailored maintenance schedule helps sustain improvements and detect recurrence early.
Surgical access is recommended when pocket depths exceed what non-surgical methods can thoroughly clean or when anatomic factors prevent effective maintenance. Flap procedures permit direct visualization and debridement of root surfaces, recontouring of bone when necessary, and reduction of pocket depths to create a more maintainable environment. The decision to proceed surgically depends on disease severity, the patient’s healing capacity, and long-term goals for the dentition.
Regenerative techniques such as guided tissue regeneration and bone grafting are used in appropriate cases to rebuild lost bone and connective tissue, improving stability and function. Modern tools, including lasers and microsurgical instruments, can reduce postoperative discomfort and enhance healing for selected procedures. Each surgical plan is customized to the patient’s anatomy, needs, and restorative objectives.
Systemic health and lifestyle choices strongly influence periodontal disease risk and treatment outcomes. Conditions like diabetes can impair healing and increase susceptibility to infection, while tobacco use and certain medications can worsen inflammation and reduce treatment effectiveness. Identifying and managing these factors is an essential part of a successful periodontal plan.
Coordinating care with medical providers helps ensure that periodontal therapy aligns with overall health management, such as blood sugar control or medication adjustments. Counseling on smoking cessation and addressing modifiable risks improve both oral and systemic outcomes. A personalized approach that considers the whole patient yields more predictable, long-term results.
Initial nonsurgical treatment is usually performed under local anesthesia to ensure comfort during scaling and root planing, and patients may experience mild soreness for a few days afterward. Postoperative instructions typically include gentle oral hygiene, short-term use of antiseptic rinses, and temporary dietary adjustments to support healing. Discomfort is generally manageable with over-the-counter analgesics and resolves as inflammation subsides.
For surgical or regenerative procedures, recovery times vary with the complexity of treatment but often include a series of follow-up visits to monitor healing and remove any sutures. Maintaining excellent home care and attending recommended maintenance appointments are critical for long-term success. Your dental team will provide a clear treatment sequence and explain expected milestones so you know what to expect at each stage.
Preventing recurrence depends on consistent daily oral hygiene and adherence to an individualized maintenance plan. Effective brushing twice daily, daily interdental cleaning with floss or interdental brushes, and periodic use of recommended antiseptic rinses reduce bacterial load and help maintain healthy pocket depths. Controlling systemic risk factors, such as smoking cessation and management of diabetes, further lowers the chance of relapse.
Regular professional cleanings and periodontal re-evaluations allow clinicians to detect early signs of recurrence and intervene before significant damage occurs. Your dental team will recommend maintenance intervals based on your risk profile, which may be more frequent than routine six-month visits for patients with a history of periodontitis. Long-term success relies on the partnership between the patient’s home care and professional preventive care.
A referral to a periodontist is considered when disease does not respond to initial therapy, when pockets continue to deepen, or when complex surgical or regenerative procedures are indicated to restore lost support. Other reasons for referral include severe bone loss, need for specialized implant planning, or medical conditions that complicate periodontal management. Early collaboration with a specialist can improve outcomes for challenging cases.
The office of Amaya Dental works with specialists when a patient’s condition requires advanced care, coordinating treatment and follow-up to maintain continuity. Referral is a step toward providing the most appropriate care, not a sign of failure, and it ensures patients have access to the full range of contemporary periodontal therapies. Clear communication between providers helps align treatment with each patient’s oral and overall health goals.
Quick Links