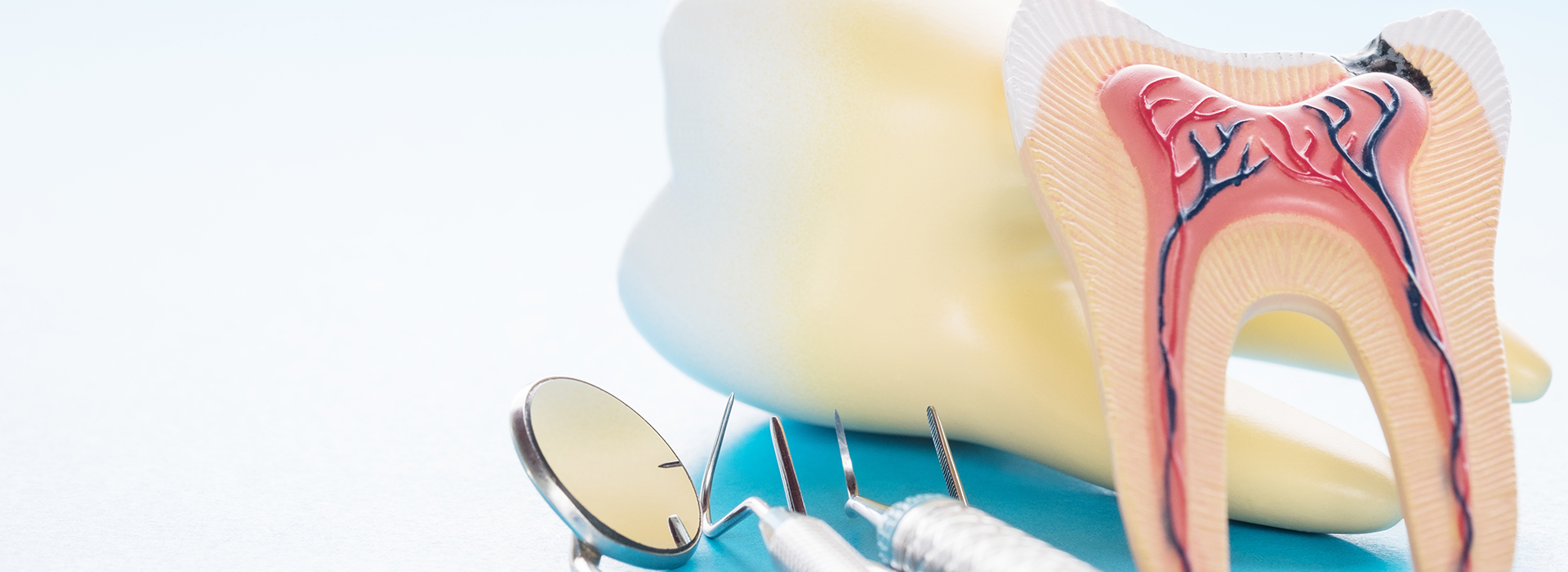
Being told you need a root canal can sound frightening, but modern endodontic care is focused on comfort, precision, and saving your natural tooth whenever possible. Root canal treatment removes the problem inside a tooth so the external structure can be preserved and restored — usually with predictable, long-lasting results.
Our offices in Miami and Pembroke Pines use up-to-date tools and techniques to make the process straightforward for patients. We prioritize clear communication and patient comfort so you understand each step and feel confident about the care you receive.
When the soft tissues inside a tooth — the dental pulp — are damaged by decay, trauma, or infection, root canal therapy offers a way to keep the tooth rather than remove it. Treating the internal tissues and sealing the canals allows the remaining tooth structure to be restored, which supports chewing, jaw alignment, and overall oral health.
Endodontic treatment has a high rate of success. With modern techniques and proper restoration after treatment, many teeth that receive root canals continue to function normally for years, often for the life of the patient. Choosing to save a tooth whenever possible helps avoid the bone loss and shifting of adjacent teeth that can follow extraction.
Deciding between extraction and root canal therapy involves considering the tooth’s condition, remaining structure, and your oral health goals. Your dentist will review imaging and perform an exam to recommend the option most likely to provide lasting function and comfort.

Inside each tooth is a chamber filled with connective tissue, nerves, and blood vessels known as the dental pulp. That tissue helps a tooth develop and, while a mature tooth can survive without it, the pulp still provides important sensory feedback. When bacteria reach the pulp through cavities or a crack, inflammation and infection can follow.
Not every toothache means a root canal is necessary, but certain signs suggest the pulp may be compromised. Sensitivity that lingers after a hot or cold stimulus, persistent aching, or a sudden change in comfort when biting can all be indicators that a deeper problem exists. Often these symptoms worsen without treatment.
Other clues include visual changes and swelling: a tooth that turns dark after an injury, gums that are puffed or tender near one tooth, or unexplained looseness are all reasons to seek evaluation. Early diagnosis gives the best chance of preserving the tooth and preventing a spreading infection.
Although symptoms are helpful, some affected teeth show little or no pain yet reveal issues on X-rays. Regular oral exams and radiographs help identify teeth that need attention before the problem becomes more complicated.
Severe or ongoing pain that does not respond to home remedies often indicates that decay or inflammation has reached the tooth’s interior and requires professional care.
Sensitivity that lingers long after exposure to temperature changes can suggest the nerve inside the tooth is irritated or damaged.
Discomfort when chewing or when pressure is applied to a tooth can point to structural damage or pulpal involvement that needs evaluation.
A tooth that becomes discolored after trauma or over time may indicate internal changes such as pulp necrosis or prior injury.
Injuries that expose the inner tooth structures can allow bacteria to enter and compromise the pulp, making treatment necessary to save the tooth.
Redness, swelling, or a small pimple-like bump on the gums adjacent to a tooth can indicate an abscess and warrants prompt dental attention.
Infection and bone loss around a tooth can reduce support and cause mobility; addressing the source often halts progression and allows healing.
Prompt evaluation and treatment make a significant difference in how predictable and successful care will be. When infection is limited to the pulp and the surrounding tissues are relatively healthy, endodontic treatment and restoration are more likely to succeed with less complication.
Delaying care can allow bacteria to spread beyond the root tip, leading to more extensive bone involvement and increased discomfort. In some cases an initially treatable tooth may become more difficult to save if left untreated, requiring more complex interventions.
Routine dental exams and radiographs often catch problems before symptoms become severe, which is why keeping up with regular visits is an important part of avoiding emergency situations and preserving long-term oral health.
If your dentist recommends endodontic treatment, scheduling it in a timely manner reduces the likelihood of worsening symptoms and supports a smoother recovery and restorative process.
Root canal therapy is a precise, methodical procedure designed to remove diseased tissue, disinfect the canal system, and seal the tooth to prevent reinfection. It typically begins with a thorough exam and X-rays to map the tooth’s unique anatomy and assess the extent of damage.
Treatment usually takes place under local anesthesia to ensure comfort. The dentist creates a small opening in the crown of the tooth to access the pulp chamber, then uses specialized instruments and irrigation to remove inflamed or infected tissue and clean the canals.
After cleaning, the canals are shaped and filled with a biocompatible material to seal the space. Some cases are completed in a single visit, while others may require two appointments depending on the tooth’s complexity or the presence of active infection.
Once root canal therapy is finished, the tooth will typically receive a permanent restoration—often a crown—to protect the remaining structure and restore full function. Sedation options are available for patients who experience significant anxiety, and your dentist can discuss which approach best fits your needs.
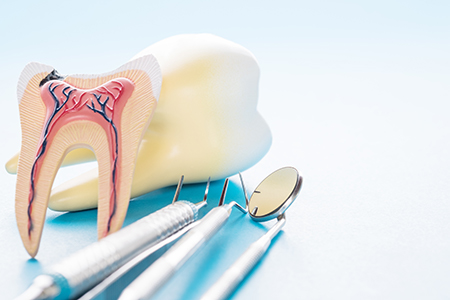
After a root canal, most patients experience relief from the intense pain that brought them in. Some mild soreness or sensitivity around the treated tooth is common for a few days as the tissues heal. Over-the-counter pain relievers and conservative self-care usually manage this discomfort effectively.
It’s important to protect the treated tooth until a permanent restoration is placed. A temporary filling is often used immediately after treatment, and the definitive crown or restoration should follow as recommended to restore strength and prevent fracture.
Complete any prescribed medications, such as antibiotics, according to your provider’s instructions. Maintain your regular oral hygiene routine, paying gentle attention to the area as it heals, and return for follow-up visits so your dentist can confirm the tooth is recovering as expected.
At Amaya Dental, we emphasize clear post-procedure instructions and available support so patients feel secure during recovery. With appropriate care, teeth treated with root canal therapy can remain functional and symptom-free for many years.
You may be numb for a few hours after your appointment. Avoid chewing or touching the treated area until normal sensation returns to prevent accidental injury.
Mild soreness is common and typically subsides within several days. Follow your dentist’s guidance on pain relief and call if symptoms worsen or persist.
If antibiotics are prescribed to address or prevent infection, take the full course exactly as directed to support healing.
A temporary filling won’t provide the same strength as a crown—avoid hard or sticky foods on that side until the permanent restoration is in place.
Continue brushing and flossing to keep the area clean and support long-term success of the treated tooth.
Restoring the tooth with an appropriate crown or filling strengthens it and reduces the chance of future complications.
Root canal therapy is a well-established treatment that can relieve pain, eliminate infection, and preserve your natural smile. If you have symptoms or concerns about a specific tooth, please contact us for more information and to arrange an evaluation.
A root canal procedure is the best way to save a tooth that has been damaged by decay or injury and preserve your natural smile. The alternative is an extraction and treatment to replace the tooth. While at times a tooth is non-restorable and an extraction is the only option, when possible, it’s best to try and save your natural tooth. With proper care, a tooth with root canal therapy can serve your smile well for many years to come.
Despite lingering myths from before the age of modern dental anesthesia and technology, having a root canal procedure today is as routine and comfortable as visiting the dentist for a filling. While the procedure is performed under local anesthesia with your tooth completely numbed, we can also discuss options in dental sedation.
Whether the symptoms of a dental infection subside after a course of antibiotics, a draining abscess provides you with some temporary pain relief, or a tooth with radiographic evidence of pathology has not yet developed symptoms, it’s essential, before an infection worsens or occurs, to have a root canal procedure performed. In this way, the tooth can be disinfected, filled, and sealed to protect your health and avoid further problems.
If you have sustained a dental injury, have a toothache, jaw pain, swelling, or are experiencing any other unusual and uncomfortable oral symptoms, contact our office immediately for care. Dental problems that have not been evaluated and treated can significantly worsen, producing more severe damage and consequences for the involved teeth, your oral health, and even your overall wellbeing. Once you get in touch with our office, our friendly and compassionate office team will get you in for care at your earliest convenience.
While some root canal procedures can be completed in one visit, others may involve 2 or 3 appointments. How long it takes depends on various factors, including active infection, the number of canals in the tooth, and the tooth’s location or anatomy.
With a success rate that exceeds 95%, root canal therapy remains the most effective procedure to save a tooth in which the inner vital tissues have been damaged. However, as with all healthcare procedures, there are a small percentage of cases where the teeth become symptomatic a second time. The good news is that many of these teeth can still be saved with root canal retreatment or a minor surgical procedure known as an apicoectomy.
The best ways to maintain a tooth with root canal therapy are to get the proper restoration required to rebuild and protect the tooth, maintain proper oral hygiene, and schedule appointments for routine dental checkups and care.
Saving a tooth with root canal therapy is a wise investment that, in the long run, is typically less costly and invasive than having the tooth extracted and replaced with a fixed bridge or implant. As far as the exact cost of care, it can vary depending on which tooth is being treated. Many dental insurance plans provide coverage for root canal therapy. At the office of Amaya Dental, we do our best to optimize your dental benefits and minimize your out-of-pocket expenses. Our staff will answer all your questions about the cost of care and discuss all your payment options.
At the office of Amaya Dental, we use the latest technology and most effective methods of care to provide precise and gentle care. Our reputation for excellence is based upon a consistent record of achieving successful treatment outcomes while providing prompt, stress-free, and convenient treatment for every type of dental need.
A root canal is an endodontic procedure used to remove infected or inflamed dental pulp from inside a tooth while preserving the external tooth structure. The treatment eliminates the source of infection, disinfects the canal system, and seals the space to prevent reinfection. When combined with an appropriate restoration, root canal therapy allows the tooth to continue functioning for many years.
Root canal therapy is focused on saving the natural tooth rather than extracting it, which helps maintain chewing function, proper bite alignment, and the health of adjacent teeth. Modern techniques and materials have made the procedure predictable and minimally invasive. Your dentist will review imaging and anatomy to determine whether root canal therapy is the best option for a given tooth.
Certain symptoms commonly suggest the dental pulp may be compromised, including lingering sensitivity to hot or cold, persistent or severe toothache, and pain when biting. Visible signs such as darkening of a tooth, swelling or tenderness of the gums near a tooth, or a small pimple-like bump on the gum can also indicate an abscessed tooth. Some affected teeth produce little or no pain but show changes on radiographs, which is why regular exams are important.
Not every ache requires a root canal, but progressive or worsening symptoms merit prompt evaluation to prevent spread of infection. Early diagnosis often improves the chances of preserving the tooth with a straightforward treatment. Your dentist will combine your symptoms with clinical exam and X-rays to make an informed recommendation.
Root canal therapy typically begins with a thorough exam and radiographs to map the tooth's anatomy and determine the extent of infection. The dentist administers local anesthesia for comfort, creates a small access in the crown, and uses specialized instruments and irrigation to remove diseased tissue and disinfect the canals. After shaping and cleaning the canals, the space is filled with a biocompatible material and sealed to prevent reinfection.
Some cases are completed in a single visit, while others require two appointments if active infection or complex anatomy is present. Following endodontic treatment, the tooth is restored with a permanent filling or crown to protect remaining structure and restore full function. Your dentist will explain expected timelines and any recommended follow-up steps based on the specific tooth involved.
Most patients report that root canal therapy is no more uncomfortable than receiving a routine filling because the procedure is performed under local anesthesia to eliminate pain during treatment. Many people experience immediate relief from the severe pain that prompted treatment once the infected tissue is removed. Sedation options are available for patients with significant anxiety to enhance comfort and reduce stress during the procedure.
Mild soreness or sensitivity for a few days after treatment is common as tissues heal, and this is usually managed with over-the-counter pain relievers and conservative self-care. If pain increases or persistent swelling occurs after treatment, contact your dental provider for evaluation. Clear post-procedure instructions and follow-up help ensure a smooth recovery and address any unexpected concerns.
The primary alternative to root canal therapy is extraction of the affected tooth, which may then be followed by options for tooth replacement such as a dental implant, bridge, or partial denture. Extraction eliminates the infected tooth but can lead to bone loss and shifting of adjacent teeth if a timely replacement is not planned. Preserving a natural tooth with root canal therapy is generally preferred when the tooth is restorable and the prognosis is good.
Deciding between saving a tooth and extracting it depends on factors like remaining tooth structure, the extent of infection, overall oral health, and patient goals. Your dentist will review diagnostic imaging and discuss the likely outcomes and long-term implications of each choice. A thoughtful evaluation helps patients select the option that best balances function, health, and durability.
With proper treatment and restoration, many teeth that undergo root canal therapy remain functional for many years and often for the life of the patient. Longevity depends on factors such as the quality of the endodontic procedure, the integrity of the final restoration, bite forces on the tooth, and the patient's oral hygiene habits. A well-fitting crown or filling that protects the remaining structure significantly improves the long-term prognosis.
Occasionally a treated tooth may require retreatment or additional procedures if persistent infection, new decay, or structural failure occurs. Regular dental exams and radiographs help monitor healing and detect issues early so timely care can be provided. Following your dentist's restoration and maintenance recommendations gives the best chance for lasting success.
After a root canal, most patients experience immediate relief from acute pain, followed by mild soreness around the treated tooth for a few days as surrounding tissues heal. Numbness from local anesthesia may persist for several hours, so avoid chewing on the treated side until normal sensation returns to prevent accidental injury. Your dentist will provide guidance on managing discomfort and any prescribed medications.
It is important to protect the treated tooth until the permanent restoration is placed; temporary fillings are not as strong as a crown and can be vulnerable to fracture. Maintain gentle oral hygiene around the area and avoid hard or sticky foods on that side until the final restoration is complete. Attend any scheduled follow-up visits so your provider can confirm healing and finalize the restorative plan.
Not every tooth is an ideal candidate for root canal therapy; the decision to save a tooth depends on the amount of remaining structure, the presence of fractures or cracks, the extent of bone and root damage, and the tooth's strategic value in the mouth. Vertical root fractures or teeth with very limited remaining tooth material may have a poor prognosis even after endodontic treatment. In such cases, extraction and replacement may provide a more predictable long-term outcome.
Your dentist will evaluate the tooth using clinical exam and radiographs and discuss realistic expectations for success and possible alternatives. When a tooth is salvageable, modern endodontic techniques can often resolve infection and restore function. If saving the tooth is unlikely to provide durable results, your provider will explain replacement options and next steps.
Preventive measures that lower the risk of pulp infection include consistent oral hygiene with twice-daily brushing and daily flossing, routine dental exams and radiographs to catch cavities early, and prompt treatment of tooth decay or cracks. Using a custom night guard if you grind your teeth and wearing a sports mouthguard during contact activities can protect teeth from structural damage that leads to pulp exposure. Early intervention for dental problems gives the best chance to avoid more invasive procedures.
Lifestyle habits such as limiting frequent sugary snacks and seeking timely dental care after trauma also reduce the likelihood of developing infections that require root canal therapy. Regular professional cleanings and risk-based recall intervals help maintain overall oral health and identify issues before they progress. Discuss personalized prevention strategies with your dental team to address specific risk factors.
Dental teams commonly offer a range of comfort measures to help anxious patients, starting with effective local anesthesia and extending to sedation options such as nitrous oxide or oral sedatives when appropriate. These approaches allow many patients to undergo endodontic treatment with minimal awareness of the procedure and greater relaxation. The choice of sedation depends on the patient's medical history, level of anxiety, and the complexity of the treatment.
Discuss your concerns with your dentist in advance so they can recommend the most suitable comfort strategy and explain what to expect before, during, and after treatment. Many practices also use calming office protocols, clear communication, and step-by-step explanations to reduce fear and build confidence. At Amaya Dental our team will work with you to identify options that support a comfortable and safe experience for root canal therapy.
Quick Links