According to the National Institute of Dental and Craniofacial Research (NIDCR), temporomandibular joint disorders (TMJ or TMD) are one of the leading causes of chronic facial pain and impaired jaw function. These problems affect millions of people and can range from brief, self-limited discomfort to persistent, life-disrupting symptoms. Understanding how the joint works and what can go wrong is the first step toward effective management.
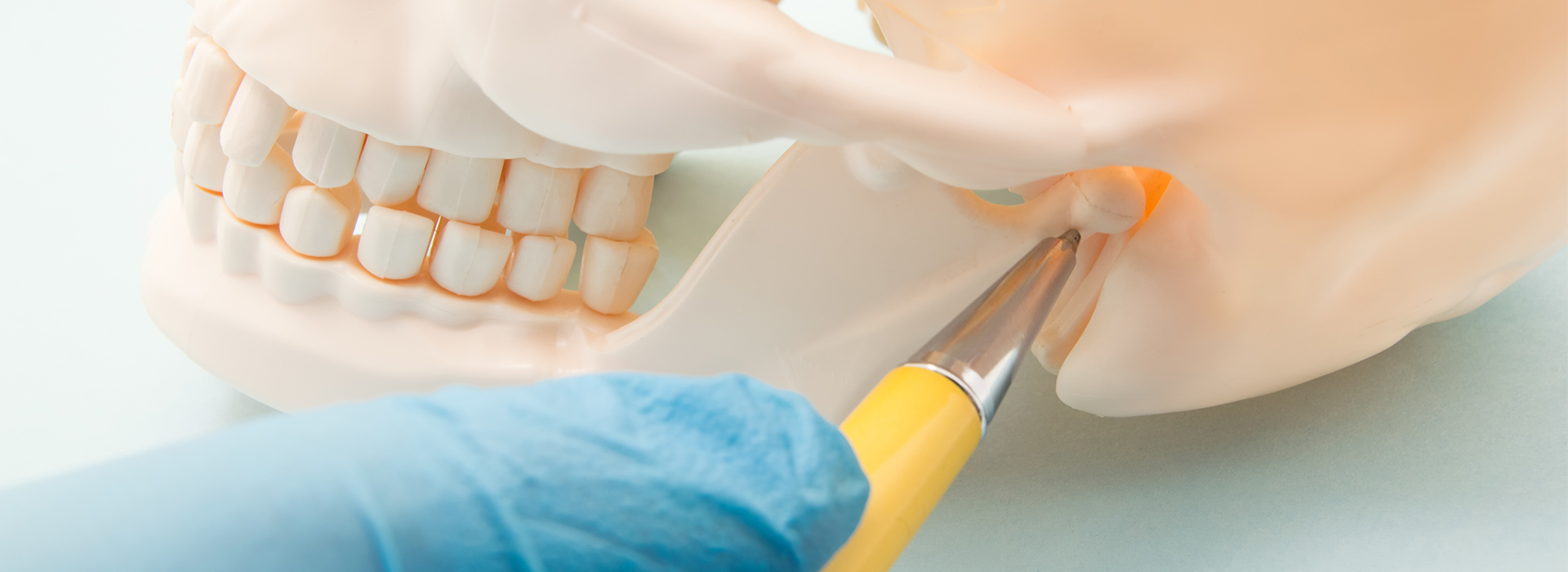
The temporomandibular joint is actually a pair of joints—one on each side of the head—where the lower jaw (mandible) meets the temporal bones of the skull. Each joint contains a lubricating disc that cushions the rounded condyle of the mandible as it moves within the socket. Muscles, ligaments and tendons surround the joint and coordinate to allow complex motions like opening, closing, sliding and rotating.
Because the TMJ must perform both hinge-like opening and closing as well as sliding and lateral movements, it is mechanically intricate and highly coordinated. That complexity makes the joint vulnerable to wear, strain, and structural problems that can manifest in many different ways. Small changes in alignment, muscle function, or joint surfaces can have outsized effects on comfort and mobility.
The relationship between teeth, bite (occlusion), and joint mechanics is also important. How the teeth meet can influence jaw position and muscle activity, and conversely, joint or muscle dysfunction can change how the bite feels. This interconnected system helps explain why TMJ disorders can present with both dental and non-dental complaints.
TMJ problems rarely have a single cause; more often they result from a combination of factors. Persistent teeth grinding or clenching (bruxism) is a frequent contributor because it places repeated stress on the muscles and joint surfaces. Acute trauma to the jaw—such as a fall or a blow—can also lead to disc displacement, fractures, or soft-tissue injury that triggers ongoing symptoms.
Inflammatory conditions and degenerative diseases can affect the joint directly. Osteoarthritis and rheumatoid arthritis may alter joint cartilage and bone, creating pain, stiffness, and limited motion. Systemic health issues that influence inflammation, pain perception, or muscle tone can also make TMJ complaints more likely or harder to resolve.
Behavioral and postural factors deserve attention as well. Chronic poor posture, particularly forward head carriage, can increase tension in neck and facial muscles and indirectly strain the TMJ. Likewise, habits such as prolonged gum chewing, biting nails, or holding objects between the teeth can perpetuate muscle overuse and discomfort.
People with TMJ disorders often report a constellation of symptoms that may seem unrelated at first. Local signs include jaw pain or tenderness, difficulty opening or closing the mouth fully, and audible clicking, popping, or grating with movement. Episodes of the jaw “locking” in an open or closed position can be alarming and may indicate mechanical displacement within the joint.
TMJ dysfunction can also produce symptoms that mimic ear or head conditions. Ear pain, a feeling of fullness in the ear, or ringing (tinnitus) are common complaints. Headaches—especially around the temples or behind the eyes—and facial pain that radiates to the neck and shoulders frequently accompany jaw problems and are often the reason patients initially seek care.
Symptom severity and pattern vary widely. Some people experience brief flare-ups that respond to conservative measures, while others live with persistent, fluctuating pain that affects sleep, mood, and daily activities. Because symptoms overlap with dental, ENT, neurologic and musculoskeletal conditions, careful evaluation is important to identify the correct source of the problem.
If symptoms interfere with eating, speaking, or restful sleep, or if they escalate suddenly after trauma, a prompt clinical assessment is recommended. Early recognition and appropriate management can reduce the risk of chronicity and help restore function more quickly.
Diagnosing TMJ disorders begins with a thorough clinical exam that assesses jaw movement, muscle tenderness, joint sounds, and how the teeth come together. The history is equally important: clinicians look for patterns such as nocturnal grinding, the onset and progression of symptoms, prior injuries, and any systemic health issues that could play a role.
Imaging can clarify structural concerns when indicated. Panoramic or cone-beam CT scans provide high-resolution views of bone anatomy, while MRI is the preferred tool to visualize the joint’s soft tissues, such as the articular disc and surrounding ligaments. These studies are used selectively, guided by the clinical picture, to inform treatment decisions and rule out other conditions.
Because TMJ disorders can arise from dental, muscular, and joint sources—or a combination—evaluation is often collaborative. Dentists, oral surgeons, physical therapists, and sometimes ENT or rheumatology specialists may be involved in complex cases to ensure a comprehensive diagnosis and coordinated care plan.
Treatment for TMJ disorders typically follows a conservative, stepwise pathway tailored to the individual. Self-care measures are the foundation: short-term soft or blended diets, limiting wide mouth opening, avoiding gum and chewy foods, and applying heat or cold can relieve acute symptoms. Stress management and sleep hygiene are frequently recommended because they can reduce muscle tension and bruxism.
Clinically supervised therapies often include custom-fit oral appliances or stabilization splints designed to reduce muscle strain and redistribute occlusal forces. Physical therapy techniques—such as guided stretching, manual therapy, and posture correction—address muscle imbalance and improve functional range of motion. In many cases, combining appliance therapy with therapy and behavioral strategies produces measurable improvement.
When conservative measures are insufficient, targeted interventions may be considered. These can include guided injections (for example, corticosteroids or other agents) to reduce localized inflammation, or occlusal adjustments and restorative dental work to optimize bite relationships when they contribute to symptoms. Orthodontic or prosthodontic solutions may play a role if dental alignment is a significant factor.
Surgical options are reserved for persistent, structural problems that do not respond to noninvasive care. Procedures range from minimally invasive arthroscopy to open joint reconstruction and are performed only after careful evaluation and discussion of risks and expected outcomes. Throughout the process, the goal is to maximize pain relief and restore comfortable, stable jaw function with the least invasive, most evidence-based approach possible.
Our team applies a personalized perspective to TMJ care, coordinating diagnostic tools and therapeutic options to build a plan that fits each patient’s needs. At Amaya Dental, we combine clinical assessment with modern imaging and conservative-first treatment planning to help people regain comfort and function in their daily lives.
If you’re experiencing jaw pain, persistent headaches related to jaw movement, or other symptoms described here, consider scheduling an evaluation. Contact us for more information and to discuss how we can help you find relief and restore healthy jaw function.
Temporomandibular joint disorders, often called TMJ disorders or TMD, encompass a group of conditions that affect the joints and muscles that control jaw movement. Each temporomandibular joint connects the lower jaw to the skull and contains a small cushioning disc that helps the jaw move smoothly during speaking, chewing and yawning. Dysfunction can arise from problems with the joint surfaces, the disc, the surrounding muscles or the coordination among these structures.
Symptoms range from occasional discomfort to persistent pain and functional limitations that interfere with daily life. Because the jaw works in close relationship with the teeth, facial muscles and neck, TMJ disorders can present with a variety of dental and non-dental complaints. Early recognition and appropriate evaluation help guide effective, individualized care.
TMJ disorders rarely have a single cause and most often result from a combination of factors. Common contributors include repetitive muscle strain from teeth grinding or clenching (bruxism), trauma to the jaw, inflammatory or degenerative joint disease and parafunctional habits such as chewing gum or holding objects between the teeth. Systemic conditions that affect inflammation, connective tissue or pain sensitivity, as well as persistent poor posture, can also increase risk.
Because small changes in alignment, muscle control or joint surfaces can disproportionately affect function, even seemingly minor events may trigger symptoms that become chronic. Identifying the mix of factors that applies to each patient is a core part of planning effective treatment. A tailored approach that addresses mechanical, muscular and behavioral contributors typically yields the best results.
Local symptoms often include jaw pain or tenderness, limited ability to open or close the mouth, and clicking, popping or grating sounds with movement. Episodes of jaw locking or the sensation that the bite is changing can be alarming signs that something within the joint or its disc is displaced or not tracking smoothly. Pain may be constant or intermittent and often worsens with chewing, yawning or prolonged mouth opening.
TMJ disorders commonly cause head and face symptoms beyond the joint itself, such as temple headaches, ear pain or fullness, and referred facial or neck pain. These overlapping complaints can mimic ear, neurologic or dental conditions, so a careful, focused evaluation is important to determine whether the TMJ is the primary source of symptoms. If daily activities, eating or sleep are affected, seeking clinical assessment is advisable.
Evaluation begins with a thorough clinical history and hands-on examination that assesses jaw movement, muscle tenderness, joint sounds and how the teeth come together. Clinicians ask about symptom patterns, grinding or clenching behaviors, prior injuries and any systemic conditions that could influence inflammation or pain. This information guides whether additional testing is needed and helps differentiate dental, muscular and joint sources of dysfunction.
When indicated, imaging studies clarify structural concerns: panoramic radiographs and cone-beam CT (CBCT) visualize bone anatomy, while magnetic resonance imaging (MRI) is the preferred method to examine soft tissues such as the articular disc and ligaments. Complex cases may benefit from coordinated care with physical therapists, oral surgeons or medical specialists to ensure a comprehensive diagnosis and an individualized treatment plan.
Initial management emphasizes conservative, reversible therapies aimed at reducing pain and restoring function. Self-care measures commonly recommended include a short soft-food diet, avoiding wide mouth opening and chewy foods, applying local heat or cold, and practicing relaxation and sleep hygiene to reduce muscle tension and bruxism. Behavioral strategies such as habit reversal for clenching and stress-management techniques are often helpful adjuncts.
Clinically supervised noninvasive options include custom oral appliances or stabilization splints to reduce muscle strain, targeted physical therapy to improve range of motion and posture, and guided exercises to rebalance muscle activity. Combining multiple conservative modalities frequently produces measurable improvement and is the standard first-line approach before considering more invasive interventions.
Custom-fit oral appliances and night guards are designed to redistribute occlusal forces, reduce muscle overactivity and protect teeth from the effects of grinding. These devices can relax hyperactive muscles, decrease joint loading during sleep and provide a more stable bite relationship that alleviates strain on the TMJ. Properly fitted appliances are adjustable and intended as part of a broader, supervised treatment plan rather than as a standalone cure.
Success depends on accurate diagnosis, device design and ongoing follow-up to assess symptom change and make necessary adjustments. In many patients, combining an oral appliance with physical therapy and behavioral strategies yields better long-term control of symptoms than any single therapy alone. Regular reassessment ensures the appliance remains appropriate as symptoms and functional needs evolve.
Physical therapy addresses the muscular and postural contributors to TMJ dysfunction through targeted exercises, manual therapy and education. Therapists work on restoring balanced muscle length and strength, improving joint mobility and correcting neck and head posture that commonly increases strain on the jaw. Techniques may include guided stretching, myofascial release, neuromuscular re-education and instruction in home exercises to maintain progress.
Integrating physical therapy with dental management—such as occlusal adjustments or oral appliance therapy—often improves functional outcomes and reduces pain recurrence. The multidisciplinary approach helps address both local jaw mechanics and related cervical or postural issues, which is particularly important when symptoms extend into the neck, shoulders or head. Ongoing communication between the dental team and therapists supports coordinated care.
Seek prompt clinical evaluation if you experience sudden, severe jaw pain, acute inability to open or close your mouth, signs of infection near the joint, or rapidly worsening symptoms following trauma. These presentations may indicate disc displacement, fracture, infection or other conditions that require timely assessment and possible urgent intervention. Persistent or progressive symptoms that interfere with eating, speaking or sleep also warrant earlier clinical review.
For complex or refractory cases, referral to specialists such as oral and maxillofacial surgeons, pain medicine physicians or rheumatologists may be appropriate, particularly when structural joint disease or systemic inflammatory conditions are suspected. Coordinated, multidisciplinary evaluation helps ensure accurate diagnosis and selection of the most appropriate advanced treatments when conservative care is insufficient.
The relationship between the bite (occlusion), teeth and TMJ is complex: changes in tooth position or how the teeth meet can influence jaw posture and muscle activity, and conversely, joint or muscle dysfunction can alter the perceived bite. While routine dental procedures do not commonly cause TMJ disorders, poorly planned extensive restorative or prosthetic work that changes occlusion without proper evaluation can contribute to muscle strain or discomfort in susceptible patients. Assessment of occlusal factors is an important component of TMJ evaluation.
When dental alignment or restorative needs appear to play a role, conservative reversible measures are considered first and restorative adjustments are carefully planned to avoid creating new problems. In cases where dental factors are a clear contributor, coordinated management between restorative dentists, orthodontists and TMJ specialists helps achieve stable, comfortable function. Communication about symptoms before, during and after dental treatment helps prevent and address potential issues promptly.
Surgical intervention is reserved for persistent, structural problems that do not respond to comprehensive conservative care and where imaging confirms correctable pathology. Options range from minimally invasive arthroscopy to open joint procedures for disc repositioning or joint reconstruction, depending on the specific anatomic issues identified. Surgery is considered only after careful evaluation of risks, benefits and alternative approaches.
Before surgery, patients typically undergo multidisciplinary assessment and trial conservative therapies to maximize nonoperative improvement. If surgery is recommended, the team discusses realistic goals, expected recovery and long-term follow-up to optimize function and minimize complications. Our team at Amaya Dental works with surgical specialists when appropriate to ensure coordinated care aligned with each patient’s diagnostic findings and treatment goals.
Quick Links